Our Dementia and Delirium Outreach Team (DDOT) helps older people who have problems with their memory or thinking, such as dementia or delirium.
We assess patients when they come into hospital and help staff understand what support they need.
We also give carers and staff clear information and training. People with dementia may come into hospital for many reasons like infections, heart problems or falls and they often need extra help.
Our team works from The Alexandra Centre at Sunderland Royal Hospital. Here, patients can take part in safe and helpful activities that can improve their wellbeing. We also run a clinic to check on people after they have had delirium.
Dementia is a collective term for over 100 diseases that affect the brain. They make it hard for a person to remember things, think clearly or make decisions. It is not a normal part of getting older, but it is more common in older people.
People with dementia may:
- Forget recent events
- Get confused about time or place
- Have trouble finding the right words
- Struggle with daily tasks
- Become worried, upset or tired more easily
Dementia gets worse over time because the brain changes. There is no cure yet, but there are treatments and support that can help people live well for as long as possible.
Delirium is a sudden change in the way a person thinks and understands what is happening around them. It can cause confusion, disorientation and sometimes fear or unusual beliefs. Delirium can be treated if it is spotted early.
People with dementia can also have delirium or depression. These conditions can make it harder to tell if someone has dementia, especially in the early stages or when they are unwell with another illness.
Listen to Chris and Claire talking more about dementia and delirium in this episode of Our People Podcast:
Living with dementia or delirium
You or someone you know might be living with dementia or delirium. If you are, it's natural to have questions.
We have added some common questions and answers below. Just click the box you'd like to know more about.
If you are worried that someone may have dementia, you should talk to them about seeing their GP.
The GP may ask some questions, do a physical check and request blood tests. This is important because other health problems can cause similar symptoms to dementia and some of these can be treated. These include low vitamin levels, an under‑active thyroid or depression.
If the GP thinks there is a memory problem, they may refer the person to a specialist memory service. Getting a diagnosis helps the person, their family and their carers get the right treatment, care and support.
Early‑onset dementia is when a person develops dementia before the age of 65.
The symptoms are similar to dementia in older adults, such as changes in memory, thinking and behaviour. But younger people may have different needs and may need different types of support.
One type linked to younger people is frontotemporal dementia. This affects the front and side areas of the brain. It can cause changes in personality, unusual behaviour or problems with planning and organising.
People with learning disabilities, especially those with Down’s syndrome, are at higher risk of getting dementia at a younger age. Symptoms can start earlier and may be harder to spot at first. This is why regular health checks should include screening for dementia.
Having dementia does not always mean you must stop driving. What matters most is whether you can drive safely.
A doctor may sometimes advise you to stop driving for a short time while tests are done. This may take a few weeks, and it is important to follow medical advice.
If you are diagnosed with dementia, you must tell the Driver and Vehicle Licensing Agency (DVLA). You can do this online (click here: Health conditions and driving) or call 0300 790 6801.
You also need to tell your car insurance company.
If you are not sure how well you can drive, you can take a special driving assessment. Mobility Centres offer these tests. Click this link to find out more: Mobility Centres
If the DVLA decides you can keep driving, they will give you a new licence. This licence usually lasts for 1 year if you have dementia. In very early dementia, it may last longer, up to 3 years. Your condition will be checked again at least once a year.
A diagnosis of dementia does not always mean you must stop working. Many people can continue working, especially in the early stages. It is a good idea to tell your employer so they can support you.
A disability employment officer at Jobcentre Plus can give helpful advice. Changes at work can also make things easier. These might include shorter hours, fewer distractions, using technology to stay organised or looking at different types of work that may suit you better.
A Life Story is a way of collecting important information about a person with dementia. It helps others understand who they are, what they enjoy and what matters most in their life. As dementia gets worse, it can be harder for someone to say what they like or dislike. A Life Story helps people meet their needs in a more personal and caring way.
How do you make a Life Story?
Family, friends or staff can help create it. It can be simple and does not need to be perfect. Many people use photos and write short notes in a book or album. You can include things like:
- Childhood memories
- Places they lived or worked
- Important people and pets
- Hobbies, routines and favourite things
Some people choose to make it on a computer and print it, or create a short presentation to play on a laptop or DVD. Some Life Stories are long and detailed, while others are short, such as a “10 things you need to know about me” page.
How is a Life Story used?
A Life Story can be used by anyone who supports the person. It can help start conversations, build trust and guide daily care. It also helps staff understand what brings comfort, joy or reassurance.
Eating a healthy and balanced diet and staying mentally, physically and socially active might help reduce the risk of developing dementia.
What support is available?
A person who has dementia, delirium or other communication difficulties can struggle with changes. This can include things like moving to a new place or meeting new people who look after them.
This is me can make things less stressful. It is a questionnaire that keeps a record of who your loved one is. You can fill it in here: This is me.
It includes things about your loved one's:
- background
- habits and routines
- communication and mobility
- likes and dislikes
It helps health and social care workers build a better understanding of them as a person. This can help them deliver care that is tailored to their needs.
Filling this in as early as possible helps and it's best to keep it up to date.
It should be filled in by whoever knows the person best. If it's possible, your loved one should be involved too.
It's important to remember that this is not a medical document.
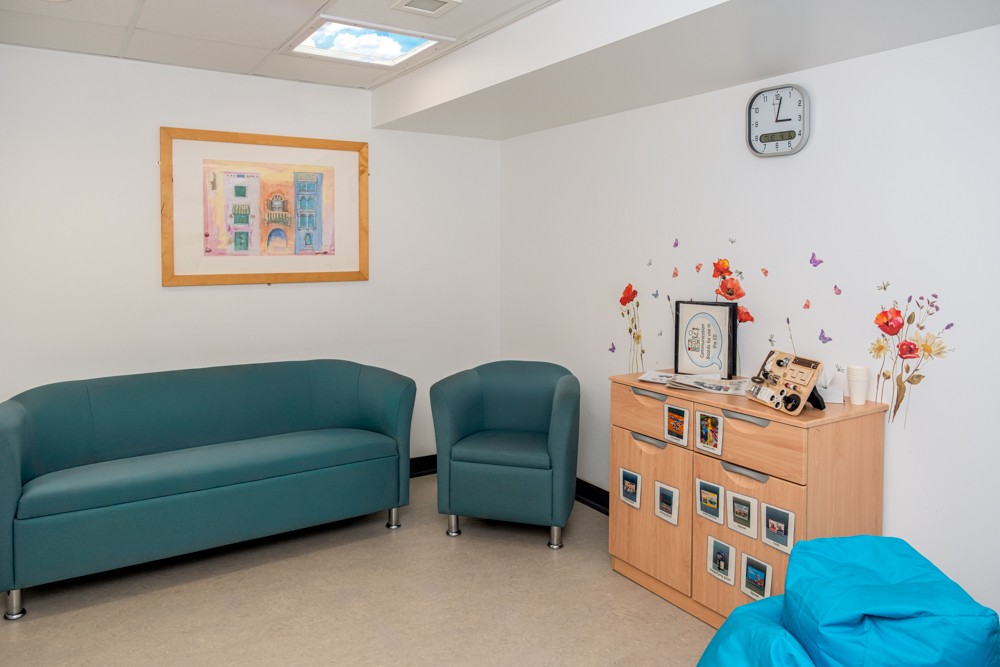
Poppy’s Place is a comfortable, quiet room in our Emergency Department (ED) at Sunderland Royal Hospital.
The room is for anyone with dementia, delirium, learning disabilities or autism.
It is a quieter, more private space for use while waiting in ED.
You can ask to use it as a reasonable adjustment. Reasonable adjustments are small changes that can help people with dementia, delirium, learning disabilities or autism while they're in hospital.
There are toilet facilities next door to the room. You can also get continence aids and equipment from ED reception.
If you would like to use the room please speak to an ED receptionist.
This is what Poppy's Place looks like:
Dementia Friends is a programme run by the Alzheimer’s Society. It aims to make life better for people with dementia by helping more people understand the condition.
A Dementia Friend is someone who has learned about dementia and wants to help others feel understood and included. They attend a short Dementia Friends information session and then choose an action they can take in their community, such as being more patient, offering support or sharing what they have learned.
There are different Dementia Friends Groups you can join. Details of these are on the Dementia Friends website.
When you’re caring for someone else, it can be easy to forget to look after yourself. But doing this can help you feel better and more able to cope with your caring role.
Caring for someone with dementia can make you feel guilty, sad, confused or angry. It can be difficult to share these feelings with someone living with dementia, leaving you feeling very alone.
It’s important to acknowledge these feelings and to remember that there’s no right or wrong way to feel. If you’re feeling anxious or depressed, or you're struggling to cope, there is help and support available to you. You can speak to your GP about this.
Carers’ groups can be a good way to get support from other carers who understand what you’re going through. You can share your own experiences and listen to others. Most groups meet regularly and might offer speakers, activities, trips and simply time to sit and chat.
You can also get in touch with the Essence Service. This is a free and dedicated service for people in Sunderland living with mild to moderate dementia and their carers. You can contact the Essence Service using the details below:
Address:
The Essence Service
Sir Thomas Allen Centre
Mill Hill Road
Doxford Park
Sunderland
SR3 2ND
Phone: 0191 522 1310
Email: essenceservice
Where can I find out more?
We are based at the Alexandra Centre. This is on E floor at Sunderland Royal Hospital.
Use the main entrance on Kayll Road. Take the stairs or the lift and follow the signs.
Our senior team in DDOT
- Divisional Director - Sheena Fish
- Directorate Managers – Joanna Finney and Beverly Wilkinson
- Nurse Consultant - Chris Cairns






